| Research Article | ||
Open Vet. J.. 2025; 15(2): 885-892 Open Veterinary Journal, (2025), Vol. 15(2): 885-892 Research Article Case fatality rate of zoonotic SARS.CoV2 and associated risk factors in the Libyan populationHafsa A. Alemam1, Abdusalam Sharef Mahmoud2*, Mouna A. Abdunnabi2, Ahlam Masaud Ellafi3, Abdurrezagh A. Elfahem4, Khaled M. Ibrahim5, Salah Edin El Meshri4 and Adam Elzghied5,61Department of Environment, Food, and Biological Application, Libyan Center for Biotechnology Research, Tripoli, Libya 2Department of Preventive Medicine, Faculty of Veterinary Medicine, University of Tripoli, Tripoli, Libya 3Department of Histology and Medical Genetics, Faculty of Medicine, University of Tripoli, Tripoli, Libya 4Department of Microbiology, Libyan Center for Biotechnology Research, Tripoli, Libya 5Department of Genetic Engineering, Libyan Center for Biotechnology Research, Tripoli, Libya 6Department of Pathology, University of Benghazi, Benghazi, Libya *Corresponding Author: Abdusalam Sharef Mahmoud. Department of Preventive Medicine, Faculty of Veterinary Medicine, University of Tripoli, Tripoli, Libya. Email: abd.mahmoud [at] uot.edu.ly Submitted: 11/11/2024 Accepted: 22/01/2025 Published: 28/02/2025 © 2025 Open Veterinary Journal
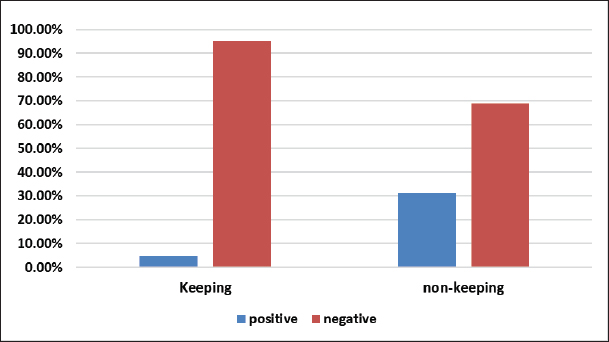
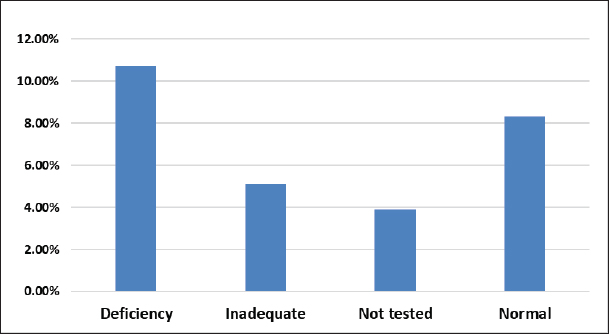
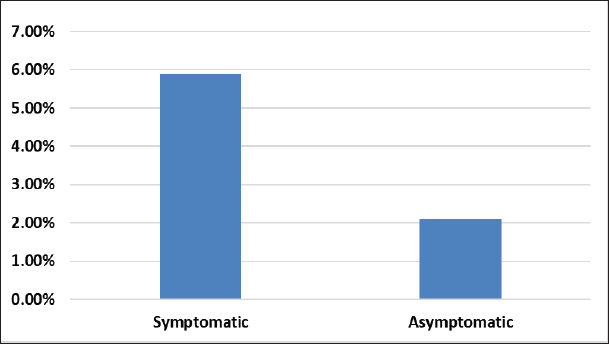
AbstractBackground: Infectious zoonotic viral respiratory diseases have dramatically emerged and reemerged globally, with high socioeconomic and public health impacts. The severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) outbreak was first reported in China as a transmissible disease among animals and humans with great universal public concern. Later, it slipped across the world as a pandemic with a high significant case fatality rate (CFR). Aim: This study was conducted to estimate the CFR and potentially associated risk factors among animals and the Libyan population. Methods: This retrospective cohort study assessed the CFR of coronavirus disease 2019 (COVID-19) and investigated the potentially associated risk factors (socio-demographic data, animal reservoir, household characteristics, and health status) among the Libyan population from July 2020 to January 2021. A total of 3,000 respiratory specimens (nasopharyngeal swabs) were screened by real-time reverse transcription polymerase chain reaction to detect SARS-CoV-2. Descriptive analyses, frequency, and percentage were measured for numerical data and numbers, and rate for qualitative data. The level of the association among variables at the significance level (p < 0.05) was investigated using SPSS version 22. Results: The present study reported a variable degree of association with the investigated risk factors included in this study: sociodemographic data, household characteristics, and health status. The overall CFR showed significant differences in vitamin D, Blood group system (ABO), health status, and comorbidity. Conclusion: The CFR seems to have been underestimated; however, our result reported a relatively high CFR in Libya, at least in the surveyed region (targeted population). The risk factors measured in this study potentially significantly influenced the CFR. Among these potential risk factors were animal welfare, vitamin D levels, the ABO system, lymphocyte count (level), and healthy status. In contrast, the results showed that other risk factors were not significantly associated with the CFR. The results highlighted the potential risk of fatalities in the country. A large set of prospective studies is required to enhance our understanding of the CFR associated with zoonotic COVID-19 in Libya. Keywords: Animal reservoir, Case fatality rate, Libya, SARS-CoV2, Zoonoses. IntroductionCoronavirus disease 2019 (COVID-19) is a highly communicable respiratory zoonotic viral disease (Contini et al., 2020). The outbreak was first reported in the Chinese territory and then spread rapidly beyond; later, the WHO declared it a public health outbreak of international concern (Chakraborty and Maity, 2020). Contact with respiratory secretions or fomites of asymptomatic and symptomatic carriers is the primary transmission route (Kulkarni et al., 2020). Coronaviruses are RNA viruses that are enclosed and found in mammals, birds, and humans. Six coronavirus species are now known to cause human disease. Four common viruses can cause respiratory symptoms: 229E, OC43, NL63, and HKU1. The other two viruses, severe acute respiratory syndrome coronavirus and Middle East respiratory syndrome coronavirus (MERS-CoV) are zoonotic and have the potential to be lethal (Li et al., 2020). The evolutionary features that enable severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) to leap from species to species (animals to people) and spillover across the globe as a pandemic has increased alarms regarding the zoonotic sources of COVID-19. However, coronaviruses are identified as zoonotic in origin, and they rapidly spread, causing high fatalities in humans. The initial infectious sources of COVID-19 are infected animals, especially bats, and rodents, and pangolins may act as intermediate hosts (Animal Reservoir) (Li et al., 2020; Shi et al., 2020). Interestingly, bats are considered native precursors of COVID-19; correspondingly, horseshoe bats of the genus Rhinolophus are considered the reservoir host of SARS-CoV, and masked palm civets (Paguma larvata) act as the intermediate host, while dromedary camels (Camelus dromedarius) act as the intermediate host that transmitted MERS-CoV to humans (Wang and Eaton 2007; Hemida et al., 2017; Zhou et al., 2020). Remarkably, the initial COVID-19 Chinese patients were related to Wuhan’s live wild and pet animal market. The viral respiratory droplets of infected individuals are an initial means of dissemination between humans and animals, especially pet felines (Cats), that can act as silent intermediate hosts of viral transmission (Kulkarni et al., 2020; Sharun et al., 2021). Studies have shown that snakes serve as intermediary hosts for the virus, transmitting it from bats to humans via homologous recombination within the S protein (Ji et al., 2020). During the COVID-19 pandemic, most citizens were extremely at risk of viral infection, especially those who traveled to Wuhan City and visited the animal market (NCDC, 2019). Genetic association with COVID-19-related mortality is usually measured by the case fatality rate (CFR), which is affected by different risk factors (Kim and Jeong, 2020; Kim et al., 2021). The COVID-19 mortality rate is calculated by dividing the number of deaths by the number of confirmed cases of COVID-19, usually ranging from 0% to 31% (Eikenberry et al., 2020; Ritchie et al., 2020). CFR varies by region and country and is significantly influenced by various factors, such as age, healthcare infrastructure, population distribution, and government public health capacities (El-Masry et al., 2021; Pang et al., 2021). Furthermore, certain preexisting medical disorders may enhance an individual’s chance of virus-related death (Natesan et al., 2024). In Libya in 2020, the CFR was estimated to be 1.40%, and the mortality rate was found to be approximately 16% (Mahmoud et al., 2021). Most epidemiological studies have reported high mortality and morbidity rates in COVID-19 cases (Daw et al., 2021). Materials and MethodsStudy design and areaThe study was conducted at the Libyan Center for Biotechnology Research from June 2020 to February 2021. Study samples (1,004) were randomly collected from men and women aged 18–70 years from different regions of Libya, according to a questionnaire designed specifically for the study. The questionnaire consists of two parts: the first part includes identifying animals, gender, age, weight, weight mass, and function. Part II covers the infection history, blood type, coronavirus-related symptoms, prevention methods, sources of infection, and treatment during infection. Samples were thoroughly examined and evaluated in the Libyan Biotechnology Research Center laboratory in Tripoli, Libya, using real-time reverse transcriptase polymerase chain reaction testing to determine the positivity or negativity of coronavirus. Statistical analysisAll relevant data were entered into Microsoft Excel spreadsheets and coded for analysis. Descriptive analyses’ frequency and percentage were measured for numerical data and number, and percentage for qualitative data using SPSS version 22. The chi-square test was used to measure the level of association among variables at a significance level of p < 0.05. Ethical approvalEthical considerations were conducted throughout the study to obtain all relevant information by providing informed consent from all tested patients. However, during this study, we followed all the criteria considering basic ethical principles in the research, like, providing anonymity and confidentiality. ResultsThe results of this study reported a variable degree of association with the investigated risk factors included in this study, sociodemographic data, household characteristics, and health status. The overall CFR was estimated at 5%. Regarding animal maintenance, results showed a significant difference p < 0.00001. Significant at p < 0.05 (Fig. 1). The results also showed that vitamin D significantly influences the CFR (p=0.032) (Fig. 2). The ABO system significantly ( p=0.00001) influences the CFR at p < 0.05 (Fig. 3). Regarding health status, the results reported (6.1%) and (2.2%) CFR among patients with and without comorbidities, respectively (Fig. 4). Health status significantly influenced the CFR (p=0.005). Likewise, occupation level, referring to the risk-based level category (low-based risk group, moderate-based risk group, and high-based risk group), had a significant (p=0.003) influence on the CFR (Fig. 5). The clinical forms of COVID-19 were estimated to be (5.9%) and (0.21%) symptomatic and asymptomatic, respectively (Fig. 6). The clinical form significantly influenced the CFR (p=0.006). Regarding the hematological parameter values (profile), the results showed variability in the significance of the association with CFR. The White Blood Cell (WBC) profile significantly ( p=0.00001) influences the CFR. However, there was no statistically significant association between CFR and other risk factors, including body mass index, smoking, infection source, Bacillus Calmette-Guérin (BCG) scar, and marital status.
Fig. 1. COVID-19 hypothesis based on keeping and non-keeping animals.
Fig. 2. CFR according to Vitamin D values.
Fig. 3. CFR based on the ABO system.
Fig. 4. CFR according to comorbidity.
Fig. 5. CFR according to occupation.
Fig. 6. CFR according to COVID-19 clinical form. DiscussionThe global unpredictable CFR of COVID-19 among different populations was significantly influenced by the variability in potential risk factors associated with the CFR of COVID-19. The present study analyzed the risk factors affecting the CFR of COVID-19 among the Libyan population. In line with various studies, there is a somewhat high CFR of COVID-19 among hospitalized patients (Mahmoud et al., 2021). However, there is variability in the frequency transmission rate of SARS-CoV-2 among different geographical regions, which might be attributable to various risk factors that increase the CFR of the COVID-19-infected population. Comparatively, the CFR (5%) reported in this study is less than that reported in other countries at the regional level (Daw, 2021; Mahmoud et al., 2023). Regarding the Vitamin D level among the study population, it significantly affects the CFR. In agreement with a previous study reporting significance associated with vitamin D content (Lau et al., 2020; Whittemore, 2020). It is well known that vitamin D in the body plays a vital role in the biological activity of body systems due to the maintenance of healthy status and functional capacities for body systems (Abushhewa et al., 2024). Therefore, vitamin D deficiency could be a predisposing factor that increases the risk of developing infectious diseases. Nevertheless, a high CFR among the population with vitamin D deficiency was of significant interest in the study population. The results revealed a significant difference in animal welfare, especially for feline species. However, there is limited evidence of the transmission of SARS-CoV-2 from humans to cats. Several studies reported evidence of SARS-CoV-2 seroprevalence in pet animals in Wuhan during the COVID-19 outbreak (Zhang et al., 2020; Michelitsch et al., 2021). The transmission of SARS-CoV-2 from species to species (trans-species spreading) suggests an increased unrestricted host range for SARS-CoV-2 (Michelitsch et al., 2023). According to phylogenic analyses, approximately 96.2% of SARS-CoV-2 has a similar genome sequence identity with Bat CoV RaTG13, indicating that SARS-CoV-2 could also originate from bats (Zhang et al., 2020). Correspondingly, sequence analysis of viral genomes from domestic cats and humans showed high similarity within the conservation region. The study results revealed variable outcomes of COVID-19 CFR in correlation with the ABO system. The AB-blood group showed a significant association with case fatality of COVID-19, whereas a lower CFR of COVID-19 was reported among the O+ blood group compared with the other blood groups. On the other hand, 0% CFR was reported among patients with O− blood group. According to published data, the ABO system might be a potential factor influencing COVID-19 clinical outcomes among hospitalized infected patients (Aljanobi et al., 2020). As a result, the variable difference in the CFR of COVID-19 in this study was reported as a consequence of the clinical outcome of the infected population. Various studies reported that those with blood group O had a lower incidence of SARS-CoV-2 infection than the non-O as compared to blood groups (Esref et al., 2020). Concerning health status, the study results showed statistical significance in association with the CFR of COVID-19. Patients with comorbidities increase the risk of mortality from COVID-19, and they are considered the most at-risk group due to the increase in the clinical severity of the infection (Deng et al., 2020; Mahmoud et al., 2023). The results showed a high CFR among patients with comorbidities compared with patients without comorbidities. Similarly, according to various studies, the CFR was higher among patients with comorbidities (Deng et al., 2020; Fang et al., 2020). Therefore, health status is an important factor affecting the CFR of COVID-19. The results of this study revealed statistically significant differences among the occupation groups. Compared to previous studies that reported substantial findings regarding CFR among different occupation groups, the high-based risk group showed a higher CFR from COVID-19 than other based-risk groups (Fang et al., 2020; Mena et al., 2021). High-risk group: health care workers without personal protective equipment are at great risk of infection with COVID-19. The proportion of symptomatic COVID-19 cases was higher than that of asymptomatic cases. The clinical form of COVID-19 has a significant influence on the CFR of COVID-19. The present study revealed significant differences in the hematological profile of infected patients. The WBC profile significantly impacted the CFR of COVID-19 among the target population. Therefore, differences in the hematological profile could be a marker for the severity and clinical outcomes of COVID-19 (Bairwa et al., 2021). Regarding the other risk factors included in this study, there was no statistically significant association between CFR and other risk factors, including body mass index, smoking, infection source, BCG scar, and marital status. ConclusionThe CFR of COVID-19 could have been underestimated; however, our results showed a relatively high CFR of COVID-19 in Libya, at least in the surveyed region (targeted population). Many risk factors analyzed in this study were significantly influenced by the CFR; among those potential risk factors were vitamin D, keeping animals, the ABO system, lymphocyte count (level), and healthy status. On the contrary, the findings indicated no significant correlation between the CFR and other risk factors, and the present results highlighted a potential risk associated with case fatality in the country. However, more research is needed to understand the role of animals as SARS-CoV-2 reservoirs. AcknowledgmentsThe authors would like to express their appreciation to the staff of the Libyan Biotechnology Research Center (BTRC), Tripoli, Libya, for their collaboration and contribution to sample testing. Conflict of interestThe authors declare no conflict of interest. FundingThe Libyan Biotechnology Research Center (BTRC), Tripoli, Libya, was acknowledged by the authors for providing funding and sample testing. Authors’ contributionsThe authors confirm their contributions to the paper as follows: Study conception and design: Hafsa A. Alemam and Abdusalam Sharef Mahmoud; data collection: Hafsa A. Alemam; analysis and interpretation of results: Abdusalam Sharef Mahmoud; Ahlam Masaud Ellafi; supervision: Abdusalam Sharef Mahmoud; Draft manuscript preparation: Abdusalam Sharef Mahmoud, Mouna A. Abdunnabi, Ahlam Masaud Ellafi, Hafsa A. Alemam, Abdurrezagh A., Khaled M. Ibrahim, Salah Edin El Meshri, and Adam Elzghied. All authors have reviewed the results and approved the final version of the manuscript. Data availabilityAll data are provided in the manuscript. ReferencesAbushhewa, M., Salem, A., Mahmoud, A., Mohsen, R. and Aqila, E. 2024. Preliminary study of vitamin D deficiency and its associated risk factors in Libya. Alq. J. Med. App. Sci. 7(1), 7–10. Aljanobi, G.A., Alhajjaj, A.H., Alkhabbaz, F.L. and Al-Jishi, J.M. 2020. The relationship between ABO blood group type and COVID-19 susceptibility in Qatif Central Hospital, Eastern Province, Saudi Arabia: a retrospective cohort study. Open J. Intern. Med. 10 (2), 232–238. Bairwa, M., Kumar, R., Beniwal, K., Kalita, D. and Bahurupi, Y. 2021. Hematological profile and biochemical markers of COVID-19 non-survivors of COVID-19: a retrospective analysis. Clin. Epidemiol. Glob. Health 11, 100770. Contini, C., Di Nuzzo, M., Barp, N., Bonazza, A., De Giorgio, R., Tognon M. and Rubino, S. 2020. The novel zoonotic COVID-19 pandemic: an expected global health concern. J. Infect. Dev. Ctries. 14, 254–264. Chakraborty, I. and Matty, P. 2020. COVID-19: migration, effects on society, global environment, and prevention. Sci. Total Environ. 728, 138882. Daw, M.A., Bouzedi A.H. and Ahmed, M.O. 2021. Epidemiological and spatiotemporal characteristics of the 2019 novel coronavirus disease (COVID-19) in Libya. Front. Public Health 9(1), 628211. Deng, G., Yin, M., Chen X. and Zeng, F. 2020. Clinical determinants of fatality in 44,672 patients with COVID-19. Crit. Care 24, 1–3. Eikenberry, S.E., Mancuso, M., Iboi, E., Phan, T., Eikenberry, K., Kuang, Y., Kostelich, E. and Gumel, A.B. 2020. To mask or not to mask: modeling the potential for face mask use by the general public to curtail the COVID-19 pandemic. Infect. Dis. Model. 5, 293–308. El-Masry, E.A., Mohamed, R.A., Ali, R.I., Al Mulhim, M.F. and Taha, A.E. 2021. Novel coronavirus disease–related knowledge, attitudes, and practices among the residents of Al-Jouf region in Saudi Arabia. J. Infect. Dev. Ctries. 15(1), 32–39. Esref, A.R.A.C., Solmaz, I., Akkoc, H., Donmezdil, S., Karahan, Z., Safak, K.A.Y.A., Mertsoy, Y., Yildirim, M.S., Nazim, E.K.I.N., Songul, A.R.A.C. and Demir, C. 2020. Association between Rh blood group and the COVID-19 susceptibility. Inte. J. Hematol. and Oncolo. 33(1), 81–86. Fang, X., Li, S., Yu, H., Wang, P., Zhang, Y., Chen, Z., Li, Y., Cheng, L., Li, W., Jia, H. and Ma, X. 2020. Epidemiological and comorbidity factors for COVID-19 severity and prognosis: a systematic review and meta-analysis. Aging (albany NY) 12(13), 12493–12493, 2013. Hemida, M.G., Elmoslemany, A., Al-Hizab, F., Alnaeem, A., Almathen, F., Faye, B., Chu, D.K., Perera, R.A. and Peiris, M. 2017. Dromedary camels and the transmission of Middle East respiratory syndrome coronavirus (MERS-CoV). Transbound. Emerg. Dis. 64(2), 344–353. Ji, W., Wang, W., Zhao, X., Zai, J. and Li, X. 2020. Homologous recombination within the spike glycoprotein of the newly identified coronavirus 2019-nCoV may boost cross-species transmission from snake to human. J. Med. Virol. 92(4), 433–440. Kim, B., Kim, S., Jang, W., Jung, S. and Lim, J. 2021. Estimation of the case fatality rate based on stratification for the COVID-19 outbreak. PLoS One, 16(2), e0246921. Kim, Y.C. and Jeong, B.H. 2020. Strong correlation between the case fatality rate of COVID-19 and the rs6598045 single nucleotide polymorphism (SNP) of the interferon-induced transmembrane protein 3 (IFITM3) gene at the population-level. Genes 12(1), 42. Kulkarni, T., Sharma, P., Pande, P., Agrawal, R., Rane, S. and Mahajan, A. 2020. COVID-19: a review of protective measures. CRST. 3(2), 244–253. Lau, F.H., Majumder, R., Torabi, R., Saeg, F., Hoffman, R., Cirillo, J.D. and Greiffenstein, P. 2020. Vitamin D insufficiency is prevalent in severe COVID-19. MedRxiv 2020-04. Li, X., Xu, S., Yu, M., Wang, K., Tao, Y., Zhou, Y., Shi, J., Zhou, M., Wu, B., Yang, Z. and Zhang, C. 2020. Risk factors for COVID-19 severity and mortality among adult COVID-19 inpatients in Wuhan. J. Allergy Clin. Immuno. 146(1), 110–118. Mahmoud, A.S., Dayhum, A.S., Rayes, A.A., Annajar, B.B. and Eldaghayes, I.M. 2021. Exploiting epidemiological data to understand the epidemiology and factors that influence COVID-19 pandemic in Libya. World J. Virol. 10(4), 156. Mahmoud, A.S., Swesi, A.R., Abeed, A.A. and Elbaz, A.K. 2023. Preliminary epidemiological investigation of COVID-19 pandemic in Alassabiea City, Libya. J. Med. Sci.18(1), 7–10. Mena, G.E., Martinez, P.P., Mahmud, A.S., Marquet, P.A., Buckee, C.O. and Santillana, M. 2021. Socioeconomic status determines COVID-19 incidence and related mortality in Santiago, Chile. Science 372(6545), eabg5298. Michelitsch, A., Allendorf, V., Conraths, F.J., Gethmann, J., Schulz, J., Wernike, K. and Denzin, N. 2023. SARS-CoV-2 infection and clinical signs in cats and dogs from confirmed positive households in Germany. Viruses 15(4), 837–838 Michelitsch, A., Schön, J., Hoffmann, D., Beer, M. and Wernike, K. 2021. The second wave of SARS-CoV-2 circulation—antibody detection in the domestic cat population in Germany. Viruses 13(6), 1009. Natesan, J., Krishnan, S. and Chopra, T. 2024. Risk factors for re-admission in Covid-19 patients from a tertiary care health system: quality control (QC) and quality improvement (QI) project. Int. J. Trop. Dis. Health 45(4), 53–60. National Center for Disease Control (NCDC). 2019. Coronavirus disease 2019 (COVID-19) [Online]. Available via https://www.cdc.gov/coronavirus/2019-ncov/about/transmission.html (Accessed 3 March 2020). Pang, M.F., Liang, Z.R., Cheng, Z.D., Yang, X.P., Wu, J.W., Lyu, K., Xi, J.J., Li, Z.J., Shi, G.Q., Zhang, Y.P. and Gao, G.F. 2021. Spatiotemporal visualization of global COVID-19 surveillance by balloon chart. Infect. Dis. Poverty 10, 1–8. Ritchie, K., Chan, D. and Watermeyer T. 2020. Cognitive consequences of the COVID-19 epidemic: collateral damage. Brain Commun 2(2), Article fcaa069 [online]. Sharun, K., Tiwari, R., Natesan, S. and Dhama, K. 2021. SARS-CoV-2 infection in farmed minks, associated zoonotic concerns, and importance of the One Health approach during the ongoing COVID-19 pandemic. Vet. Q. 41(1), 50–60. Shi, P., Dong, Y., Yan, H., Zhao, C., Li, X., Liu, W., He, M., Tang, S. and Xi, S. 2020. Impact of temperature on the dynamics of the COVID-19 outbreak in China. Sci. Total Environ. 728(1978), 138890. Wang, L.F. and Eaton, B.T. 2007. Bats, civets and the emergence of SARS. Wildlife and emerging zoonotic diseases: the biology, circumstances and consequences of cross-species transmission. Curr Top Microbiol Immunol. 315, 325–344. Whittemore, P.B. 2020. COVID-19 fatalities, latitude, sunlight, and vitamin D. Am. J. Infect. Control 48, 1042–1044. Zhang, Q., Zhang, H., Gao, J., Huang, K., Yang, Y., Hui, X., He, X., Li, C., Gong, W., Zhang, Y. and Zhao, Y. 2020. A serological survey of SARS-CoV-2 in cat in Wuhan. Emerg. Microbes & Infect 9(1), 2013–2019. Zhou, F., Yu, T., Du, R., Fan, G., Liu, Y., Liu, Z., Xiang, J., Wang, Y., Song, B., Gu, X. and Guan, L. 2020. Clinical course and risk factors for mortality among adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. The Lancet, 395(10229), 1054–1062. | ||
| How to Cite this Article |
| Pubmed Style Alemam HA, Mahmoud AS, Abdunnabi MA, Ellafi AM, Elfahem AA, Ibrahim KM, Meshri SEE, Elzagheid A. Case fatality rate of zoonotic SARS.CoV2 and associated risk factors in the Libyan population. Open Vet. J.. 2025; 15(2): 885-892. doi:10.5455/OVJ.2025.v15.i2.37 Web Style Alemam HA, Mahmoud AS, Abdunnabi MA, Ellafi AM, Elfahem AA, Ibrahim KM, Meshri SEE, Elzagheid A. Case fatality rate of zoonotic SARS.CoV2 and associated risk factors in the Libyan population. https://www.openveterinaryjournal.com/?mno=228265 [Access: January 25, 2026]. doi:10.5455/OVJ.2025.v15.i2.37 AMA (American Medical Association) Style Alemam HA, Mahmoud AS, Abdunnabi MA, Ellafi AM, Elfahem AA, Ibrahim KM, Meshri SEE, Elzagheid A. Case fatality rate of zoonotic SARS.CoV2 and associated risk factors in the Libyan population. Open Vet. J.. 2025; 15(2): 885-892. doi:10.5455/OVJ.2025.v15.i2.37 Vancouver/ICMJE Style Alemam HA, Mahmoud AS, Abdunnabi MA, Ellafi AM, Elfahem AA, Ibrahim KM, Meshri SEE, Elzagheid A. Case fatality rate of zoonotic SARS.CoV2 and associated risk factors in the Libyan population. Open Vet. J.. (2025), [cited January 25, 2026]; 15(2): 885-892. doi:10.5455/OVJ.2025.v15.i2.37 Harvard Style Alemam, H. A., Mahmoud, . A. S., Abdunnabi, . M. A., Ellafi, . A. M., Elfahem, . A. A., Ibrahim, . K. M., Meshri, . S. E. E. & Elzagheid, . A. (2025) Case fatality rate of zoonotic SARS.CoV2 and associated risk factors in the Libyan population. Open Vet. J., 15 (2), 885-892. doi:10.5455/OVJ.2025.v15.i2.37 Turabian Style Alemam, Hafsa A., Abdusalam Sharef Mahmoud, Mouna A. Abdunnabi, Ahlam Masaud Ellafi, Abdurrezagh A. Elfahem, Khaled M. Ibrahim, Salah Edin El Meshri, and Adam Elzagheid. 2025. Case fatality rate of zoonotic SARS.CoV2 and associated risk factors in the Libyan population. Open Veterinary Journal, 15 (2), 885-892. doi:10.5455/OVJ.2025.v15.i2.37 Chicago Style Alemam, Hafsa A., Abdusalam Sharef Mahmoud, Mouna A. Abdunnabi, Ahlam Masaud Ellafi, Abdurrezagh A. Elfahem, Khaled M. Ibrahim, Salah Edin El Meshri, and Adam Elzagheid. "Case fatality rate of zoonotic SARS.CoV2 and associated risk factors in the Libyan population." Open Veterinary Journal 15 (2025), 885-892. doi:10.5455/OVJ.2025.v15.i2.37 MLA (The Modern Language Association) Style Alemam, Hafsa A., Abdusalam Sharef Mahmoud, Mouna A. Abdunnabi, Ahlam Masaud Ellafi, Abdurrezagh A. Elfahem, Khaled M. Ibrahim, Salah Edin El Meshri, and Adam Elzagheid. "Case fatality rate of zoonotic SARS.CoV2 and associated risk factors in the Libyan population." Open Veterinary Journal 15.2 (2025), 885-892. Print. doi:10.5455/OVJ.2025.v15.i2.37 APA (American Psychological Association) Style Alemam, H. A., Mahmoud, . A. S., Abdunnabi, . M. A., Ellafi, . A. M., Elfahem, . A. A., Ibrahim, . K. M., Meshri, . S. E. E. & Elzagheid, . A. (2025) Case fatality rate of zoonotic SARS.CoV2 and associated risk factors in the Libyan population. Open Veterinary Journal, 15 (2), 885-892. doi:10.5455/OVJ.2025.v15.i2.37 |